Rigshospitalet — AI Virtual Assistant for Preoperative Thyroid Surgery
Bridging the information gap: AI in healthcare
Rigshospitalet recognized that patients often struggle to access or understand critical information about their upcoming procedures. Important information is too often overheard or misunderstood by patients affecting their experiences, quality of treatment, and usage of hospital resources negatively. To address these challenges, the hospital sought to improve the preoperative experience for thyroid cancer patients within their ENT department.
An AI virtual assistant for patient support
2021.AI collaborated with Rigshospitalet to develop and implement a Virtual AI Assistant, a language model-based solution designed to answer patient questions about their upcoming thyroid surgery. Trained on clinically approved data and programmed to avoid sensitive topics like diagnosis or prognosis, the Virtual AI Assistant serves as a reliable source of information.
Building trust with Responsible AI
The project team prioritized clinical, governance, and security standards, as well as responsible AI principles, throughout development. Rigshospitalet’s surgeons actively participated in testing the Virtual AI Assistant, ensuring its responses aligned with their expertise and the hospital’s specific procedures. A virtual assistant (LLM) based on key information from clinical staff, combined with governance and transparency to ensure accuracy and builds trust and confidence that the virtual assistant acts in line with hospital values and interests.
Transforming the patient experience with AI
The Virtual AI Assistant will bring significant improvements in patient care at Rigshospitalet:
Improved patient preparation: The Virtual AI Assistant gives patients instant access to accurate and relevant information, enhancing their understanding of the surgery and reducing anxiety.
Health equality: The Virtual AI Assistant provides information in various formats, promoting equitable access to healthcare information for all patients.
Efficient use of resources: The Virtual AI Assistant reduces the burden on healthcare staff, allowing them to focus on more complex patient needs, improving patient experience and quality of the treatment, and hospital efficiency. On top, it fuels innovation.
With the help of AI, we can provide support and guidance even outside of our regular opening hours. The purpose is to create patient-centeredness, security, and tranquility for the patient, their loved ones, and ourselves as healthcare providers.Mads Klokker, Head of ENT Head & Neck Surgery and Audiology, Rigshospitalet
Prioritizing safety and transparency with Responsible AI in healthcare
Patient safety remains the most important thing. The Virtual AI Assistant only references clinically approved data sources, which are clearly listed with each response. All interactions with the Virtual AI Assistant are logged for full transparency and traceability.
The collaboration between Rigshospitalet and 2021.AI highlights the potential of AI to revolutionize healthcare. The Virtual AI Assistant is a powerful example of how AI can be used to improve patient experience, promote health equity, and optimize efficiency in hospital operations.
The Problem: Hidden Operational Leakage
What we discovered is that surgical inefficiency is rarely clinical. It is informational.
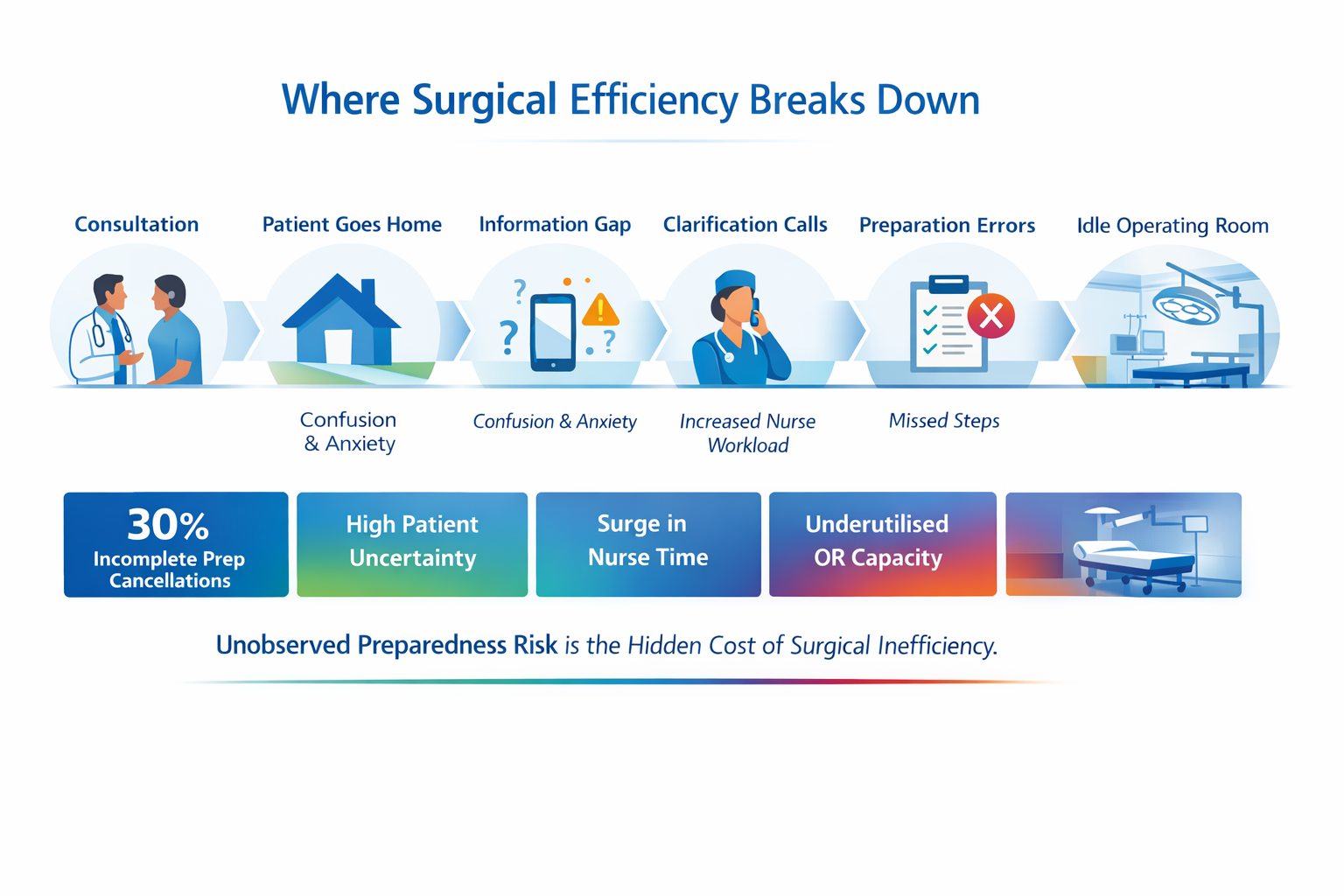
When a patient leaves consultation, they enter a high-uncertainty phase. Instructions are partially remembered. Online searches introduce conflicting information. Anxiety increases. Nurses receive clarification calls. Occasionally, preparation steps are missed.
By the time surgery day arrives, the disruption is already embedded in the system.
Every cancellation represents idle capital, sunk staffing cost, and lost throughput.
This infographic shows the invisible leakage between consultation and surgery. The issue is not clinical capability. It is unobserved preparedness risk.
If we can measure and predict that risk, we can prevent it.
The Platform: Patient Concierge Architecture
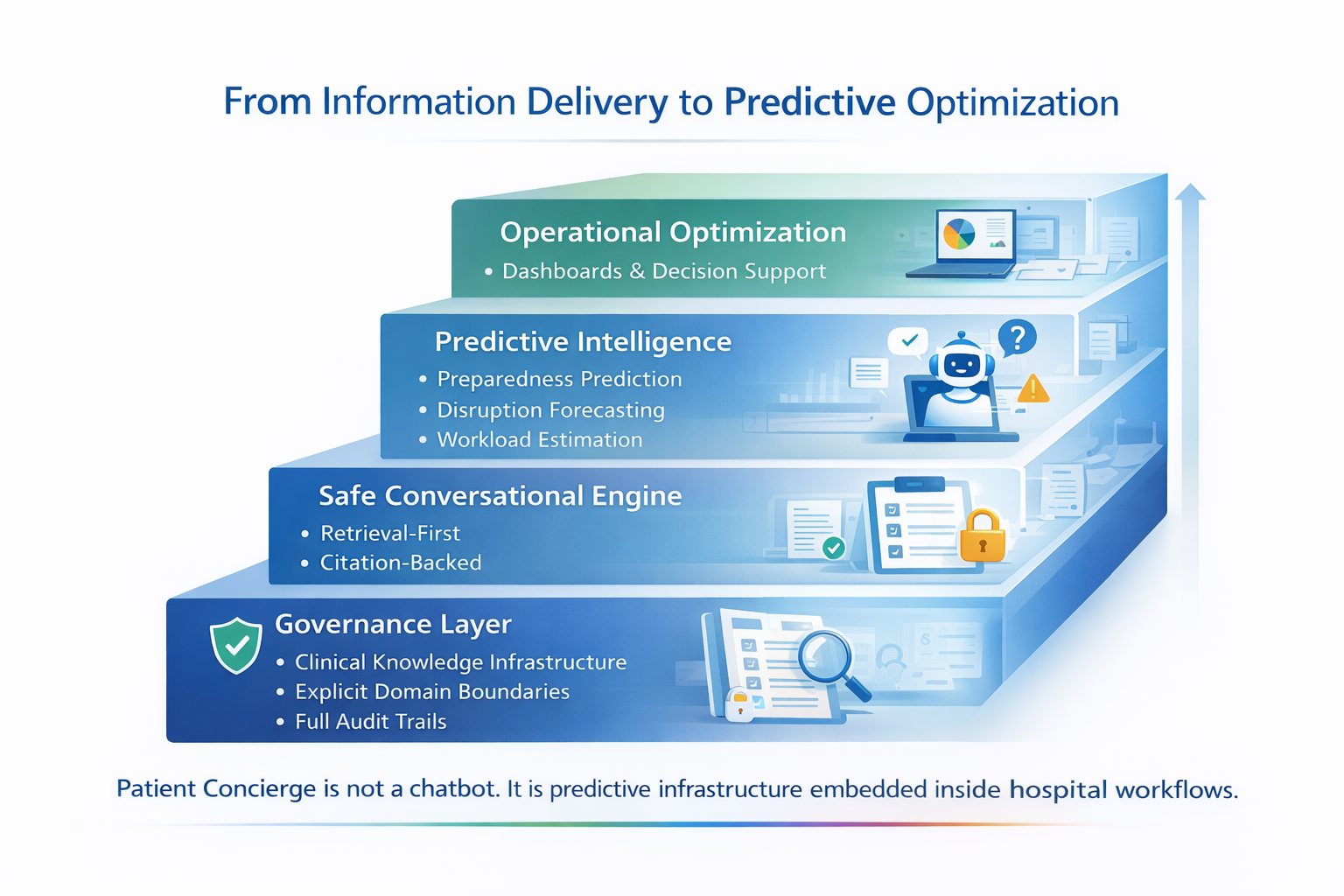
Patient Concierge is built as layered infrastructure.
At the base is governance. Clinical content is structured, approved, version-controlled, and audit-ready.
On top of that sits a safe conversational engine. It is retrieval-constrained, citation-backed, and domain-contained. It does not diagnose. It does not speculate.
Above that is the predictive intelligence layer. This is where behavioral data becomes risk modeling — preparedness prediction, disruption forecasting, workload estimation.
At the top sits operational optimization — dashboards and decision support for clinical leaders.
The key message here is this: Patient Concierge is not a chatbot. It is predictive infrastructure embedded inside hospital workflows.
The Predictive Intelligence Flywheel
This is the engine.
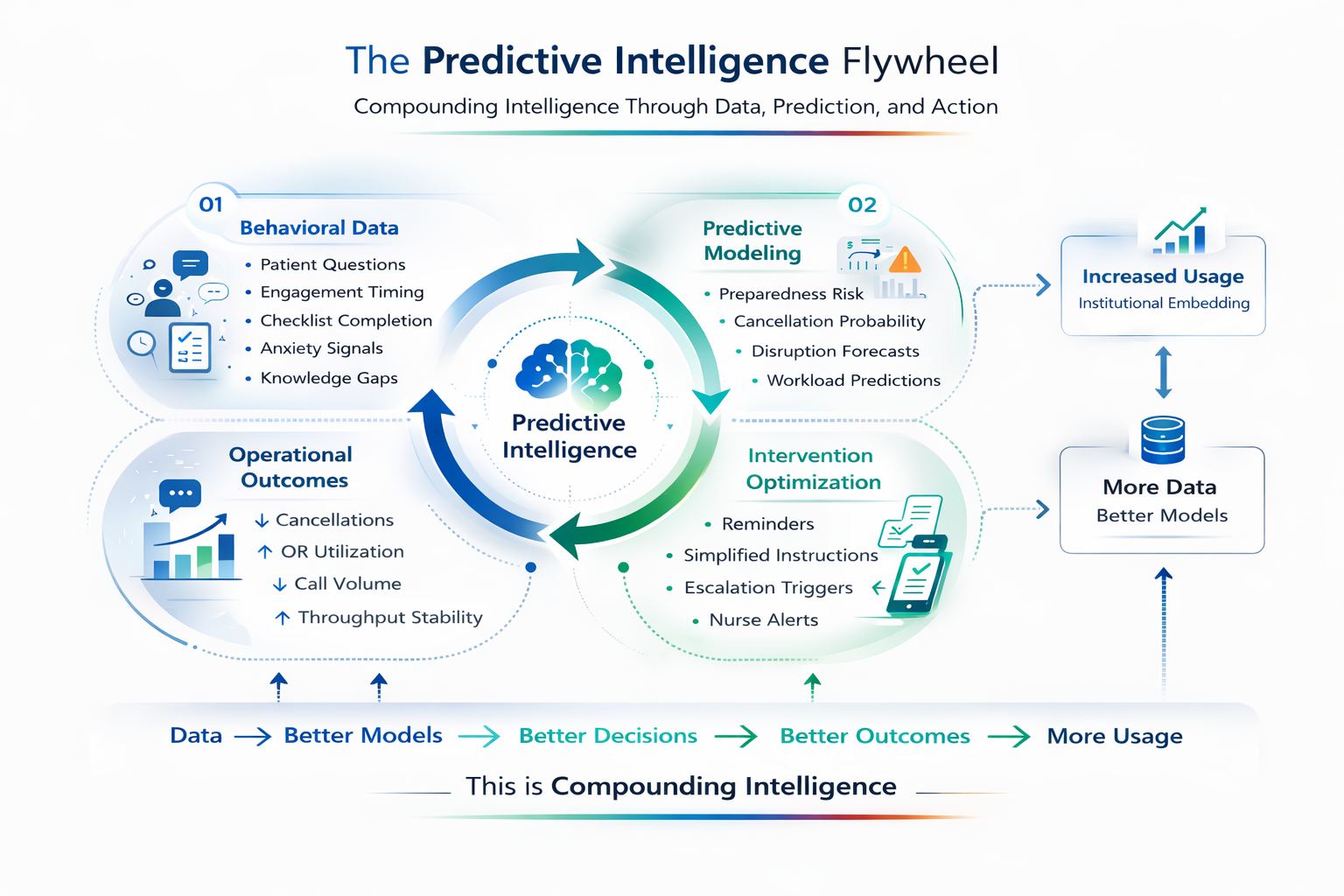
First, we observe behavioral data — how patients engage, when they ask questions, what they misunderstand.
Second, we build predictive models — who is likely to be unprepared, where disruptions will occur.
Third, we deploy targeted interventions — reminders, simplifications, escalation triggers.
Fourth, we measure outcomes — cancellation rates, workload reduction, throughput stability.
Those improved outcomes increase institutional reliance and usage.
And more usage generates more behavioral data.
Data improves models. Models improve decisions. Decisions improve outcomes. Outcomes increase usage.
This is compounding intelligence.”
Safety-First AI Framework
In healthcare, prediction without governance is unacceptable.
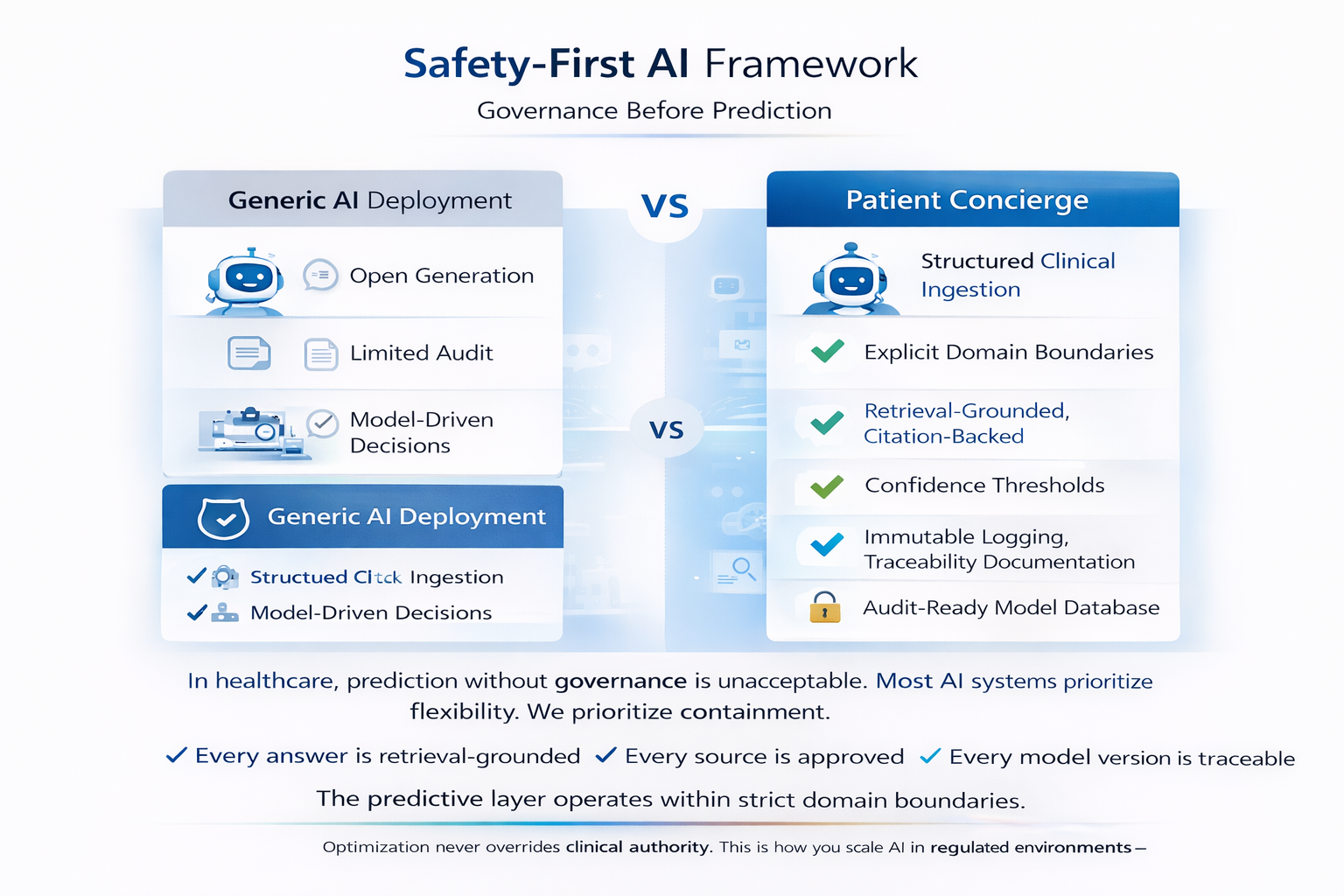
Most AI systems prioritize flexibility. We prioritize containment.
Every answer is retrieval-grounded. Every source is approved. Every interaction is logged. Every model version is traceable.
The predictive layer operates within strict domain boundaries.
Optimization never overrides clinical authority.
This is how you scale AI in regulated environments — governance first, prediction second.
Preparedness Risk Model
Patients reveal readiness through behavior.
Repeated clarification questions. Delayed engagement. Anxiety language. Checklist non-completion. Late-stage question spikes.
These signals form a preparedness profile.
Our model converts these signals into a risk score — low, medium, or high probability of incomplete preparation.
If risk crosses threshold, the system intervenes.
A reminder is sent. Instructions are simplified. A nurse is alerted.
Instead of reacting to cancellations, we predict and prevent them.
Operational Impact Dashboard
This dashboard converts prediction into operational clarity.
On the left, you see historical volatility — cancellation variance, OR underutilization, unpredictable call spikes.
On the right, after deployment, risk is quantified in advance.
Leaders can see preparedness distribution across upcoming surgeries.
They can forecast cancellation probability seven to fourteen days ahead.
They can anticipate staffing demand.
This transforms uncertainty into manageable probability.
Economic Model
Hospitals are capital-constrained systems.
Operating rooms are fixed assets. Staff are scheduled in advance.
Effective throughput equals scheduled surgeries multiplied by preparedness rate.
If preparedness improves by even a few percentage points, capital utilization rises significantly — without building new facilities.
In parallel, nurse hours previously spent on repetitive clarification are reallocated to higher-value care.
Patient Concierge increases total factor productivity.
It does not add capacity. It amplifies existing capacity.
Institutional Embedding
This is the evolution pathway.
Phase one establishes safe information infrastructure.
Phase two introduces preparedness prediction.
Phase three integrates operational forecasting.
Phase four becomes autonomous patient flow optimization.
With each phase, more data improves prediction. Better prediction improves decisions. Better decisions increase adoption.
Early adoption creates intelligence advantage.
The system becomes embedded into governance and operations.
Strategic Insights
There are five critical insights.
First, cancellations often originate in informational breakdowns, not clinical complexity.
Second, behavioral interaction data is a leading indicator of disruption.
Third, prediction improves not only efficiency but institutional confidence.
Fourth, hospitals are capacity-constrained. Small risk reductions have outsized economic impact.
Fifth, governance architecture is a prerequisite for scaling predictive intelligence in healthcare.
These insights guided product design.
The Transformation
Traditionally, hospitals operate reactively.
Consult. Inform. Hope. React to disruption.
Patient Concierge shifts the system to a learning loop.
Observe. Predict. Intervene. Measure. Learn.
Each cycle reduces uncertainty.
Each cycle compounds intelligence.
Over time, the hospital becomes a continuously improving operational system.
This is the transformation — from reactive service delivery to predictive, intelligence-driven care infrastructure.